New compound stops common complications after intestinal surgery
Liver damage, weight loss after bowel resection prevented by drug, mouse study shows
 Ayoung Kim, Daniel Lee, Bernd Zinselmeyer
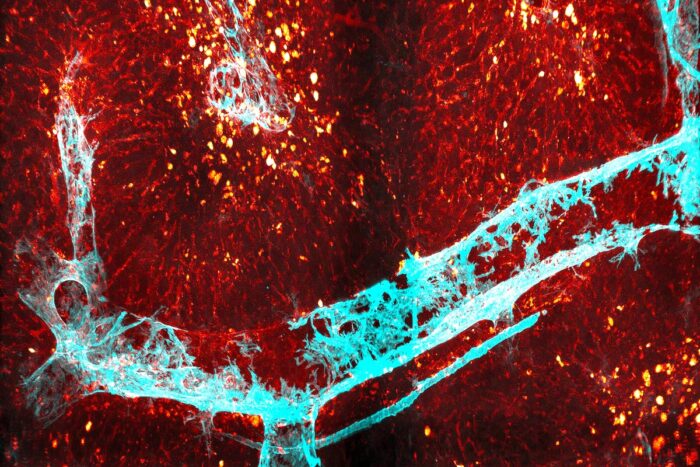
Ayoung Kim, Daniel Lee, Bernd ZinselmeyerAfter surgery to remove part of the small intestine in a mouse, normal liver tissue (red) is replaced by scar tissue (yellow-orange), which impairs the organ’s ability to function. The cyan color shows smooth muscle actin, a protein that indicates liver cells’ response to damage. Researchers at WashU Medicine made and tested a compound that protects the liver from this complication.
When parts of the small intestine are diseased or die, the treatment can involve surgically removing the affected tissue. Although lifesaving, the procedure — referred to as a radical small bowel resection — can lead to long-term liver damage and even failure, requiring a liver transplant. There are no medications to prevent or manage this serious complication that’s been reported to affect up to 15% of patients after small bowel resection.
Now, researchers at Washington University School of Medicine in St. Louis have synthesized and tested a new compound in mice that shows promise in protecting the liver from damage and improving nutrient absorption after small bowel resection. They also found that the drug works only on the gastrointestinal tract, helping to avoid side effects in other parts of the body.
The study is published March 6 in Gastroenterology.
“Our goal is to advance a therapeutic drug capable of preserving liver function and mitigating the necessity for liver transplants in people who’ve undergone small bowel surgery,” said Gwendalyn Randolph, PhD, the study’s senior author and the Emil R. Unanue Distinguished Professor of Immunology in the WashU Medicine Department of Pathology & Immunology. “This study offers a promising pathway for developing such a treatment.”
Protecting the liver through the gut
Among those treated with small bowel resection are premature infants with necrotizing enterocolitis, a serious gastrointestinal illness that requires surgery to remove the dying intestinal tissue. But the surgery results in short bowel syndrome, a condition characterized by shortened intestines and difficulty absorbing nutrients. Children with this condition often require the long-term use of a feeding pump to deliver nutrients directly into a vein. They also are at high risk for liver disease and sometimes need a liver transplant later in life.
The late Brad Warner, MD, a pediatric surgeon and researcher at WashU Medicine who specialized in gastrointestinal surgery in children, dedicated his research to improving outcomes for short bowel syndrome. In a study he collaborated on with Randolph, published in 2021, they found that a harmful substance made by gut bacteria travels to and causes damage to the liver after small bowl resection surgery. But they also observed that high-density lipoprotein, or HDL — often referred to as “good” cholesterol — can act as a protective shield that prevents gut-derived substances from harming the liver.
In the new study, on which Warner is a co-author, the researchers focused on a class of drugs, called liver X receptor agonists, that increase HDL production in the liver and intestines. Earlier studies of drugs in this class found that those that act on the whole body (systemic liver X receptor agonists) led to severe side effects. So, the research team set out to test a “gut-restricted” liver X receptor agonist — one that would affect only the intestines and not the rest of the body. They used a compound initially identified by a pharmaceutical company but never developed commercially; it was synthesized for this study by Bahaa Elgendy, PhD, an associate professor of anesthesiology at WashU Medicine and a co-author on the study who has specialized expertise in medicinal chemistry.
The researchers found that the new compound, named WUSTL0717, went to and stayed in the intestines when orally administered to mice.
They then tested whether WUSTL0717 could protect against the irreversible weight loss that commonly follows small bowel resection. They found that the drug improved nutrient absorption and aided in weight gain when administered to mice three weeks after small bowel resection, compared to untreated mice.
The researchers also found that the drug protected the liver from fibrosis — the accumulation of scar tissue that impairs liver function. Mice with resected bowels that were treated with WUSTL0717 had reduced collagen, a key component of scar tissue, in their livers compared with untreated mice or mice that underwent a sham surgery that cuts the small intestine and immediately reconnects it without removing any tissue. A genetic analysis also revealed a decrease in the activity of genes associated with fibrosis, including genes responsible for the accumulation of collagen, in the livers of treated mice.
“Our future goal is to create the next generation of tissue-specific therapies that preserve therapeutic benefit while reducing unintended systemic effects,” said Elgendy, whose research aims to create treatments that specifically activate the LXR receptor only in the tissues where they’re needed, to improve the effectiveness and reduce the side effects of current LXR-based therapies. “This precision-based strategy allows us to revisit important biological targets that were previously considered too challenging to develop safely.”
The researchers have worked with WashU’s Office of Technology Management (OTM) to file a patent for the use of WUSTL0717 to treat short bowel syndrome. Their next study will look at whether the compound still protects the liver with the added stress of intravenous nutrition, as the long-term use of this feeding method has adverse effects on the liver.
“The absence of therapies for patients with short bowel syndrome has profound implications for their long-term health,” said Colin A. Martin, MD, the Brad and Barbara Warner Endowed Professor of Surgery at WashU Medicine, a co-author on the study and a pediatric surgeon who treats children with gastrointestinal problems. “These preclinical findings represent a crucial leap forward in our goal of developing a treatment that safeguards liver function and improves nutrient absorption, enhancing the quality of life for patients affected by short bowel syndrome.”