WashU Medicine honors focused excellence with far-reaching impact
Faculty clinicians and researchers receive Dean’s Impact Awards
 Carol Green/WashU Medicine
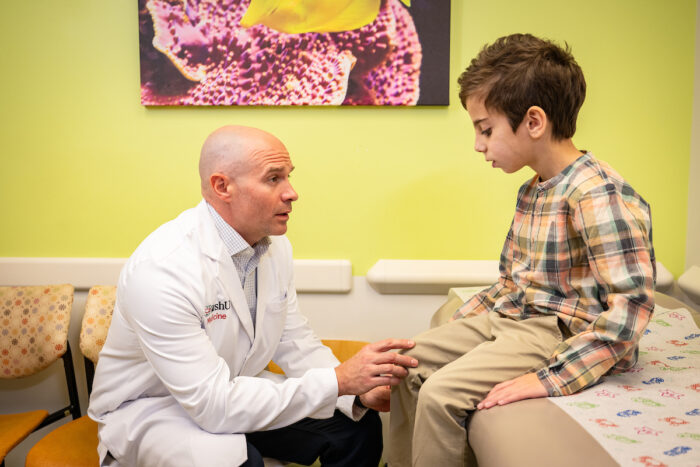
Carol Green/WashU MedicineJacob AuBuchon, MD, an associate professor of anesthesiology at WashU Medicine, treats a pediatric patient suffering from pain. AuBuchon was one of 58 faculty honored in April with Dean’s Impact Awards for focused excellence. “Pain can quietly derail a child’s entire developmental trajectory,” he said. “The good news is that they can often be treated successfully.”
WashU Medicine’s 2026 Dean’s Impact Awards recognize scientists who probe the most basic elements of life and clinicians who translate those insights into care for patients facing critical health challenges.
“This year’s theme, ‘Focused Excellence,’ highlights the brilliance of these two ends of the academic medicine spectrum,” said David H. Perlmutter, MD, executive vice chancellor for medical affairs, the Spencer T. and Ann W. Olin Distinguished Professor and the George and Carol Bauer Dean of WashU Medicine. “The magic of WashU Medicine lies in the cross-pollination between those different modes of focus — basic discoveries in the lab influencing physicians’ work and, ultimately, reaching the bedside as therapies that profoundly change human health.”
The 58 honorees recognized in April represent all 21 of WashU Medicine’s academic departments. Among those honored are a pediatric anesthesiologist who treats children’s pain as an urgent problem to be solved; a developmental biologist who studies tiny zebrafish to unravel how a spinal cord injury may one day heal itself in humans; and a rheumatologist who excels in communication with her patients to ensure they are well-informed partners in their care.
“WashU Medicine is built on the understanding that deep commitment to a chosen domain is the hallmark of exceptional faculty,” said Renée A. Shellhaas, MD, senior associate dean for faculty promotions and career development at WashU Medicine, who spearheads the awards. “This year, we are proud to honor clinicians and scientists whose devoted pursuit of focused excellence is a testament to what becomes possible when remarkable ability is matched with enduring purpose.”
Perlmutter and Shellhaas established the Dean’s Impact Awards in 2023 to recognize faculty who demonstrate the highest level of professionalism and deliver exceptional results across WashU Medicine’s missions of patient care, research and education. Each year, the awards spotlight a different area of emphasis. Past themes included extraordinary responses to the pandemic, excellent mentorship, and leadership in community engagement.
Read how three WashU Medicine faculty members honored with this year’s Dean’s Impact Awards exemplify focused excellence:
Jacob AuBuchon, MD
Not a day goes by that Jacob AuBuchon, MD, doesn’t ponder pain. Not his own per se, but rather the chronic cramping, throbbing, burning, pinching, tingling, stinging, chafing and aching pains that studies say afflict one in five children and adolescents.
AuBuchon, an associate professor in the Department of Anesthesiology, specializes in treating kids who suffer from pain. As director of pediatric pain management at St. Louis Children’s Hospital, he oversees the pain management clinic, acute pain inpatient services and regional anesthesia.
“Pain can quietly derail a child’s entire developmental trajectory,” AuBuchon said. “Yet a misperception exists that children don’t feel pain like adults do. This can cause their symptoms to be minimized or misattributed as being purely from stress or moodiness. The good news is that they can often be treated successfully.”
The WashU Medicine Pediatric Pain Management Clinic — the only one in the region — offers specialized care from a multidisciplinary team that includes psychologists and physical therapists who can help lessen pain, often in conjunction with non-addictive medications. Among the conditions treated are headaches; gastrointestinal issues; connective tissue and autoimmune disorders; genetic conditions such as sickle cell disease; diseases related to cancer; herniated discs; broken bones and strained muscles.
AuBuchon is widely praised for tripling the number of patients treated at the pediatric pain clinic over a 10-year period.
Primarily trained at WashU Medicine, AuBuchon launched a new fellowship track with a focus on pediatric pain, ensuring the longevity of the clinic through the rigorous education and mentorship of future leaders.
“When I was in middle school, I developed chronic knee pain,” AuBuchon recalled. “I wonder if subconsciously, my experience drew me into pediatric pain management. I remember my doctor telling me I was fine and I should return to my normal activities. I suppose I wanted to give kids a compassionate clinical team that takes their pain seriously and helps them to live active, pain-free lives.”
Mayssa H. Mokalled, PhD
Twelve years ago, when considering how to approach research on injuries to the human nervous system, Mayssa H. Mokalled, PhD, decided to flip the script.
Mokalled, an associate professor of developmental biology, had analyzed dozens of studies about cellular complications that often occur after a traumatic spinal cord injury, as well as potential ways to overcome life-changing damage. Many people who survive spinal cord injuries experience lifelong health problems such as paralysis, physical deformity and loss of basic body functions including urination and bowel elimination.
 Carol Green/WashU Medicine
Carol Green/WashU Medicine“I was riding my bike thinking about how we could regenerate the spinal cord in humans,” Mokalled recalled. “It occurred to me that instead of asking what goes wrong in the nerve cells after spinal cord injury, I decided to ask what goes right. We know that in nature, there are animals that can recover from paralysis caused by spinal cord injury because the nerve cells in their spinal cords can regenerate.”
Those animals include axolotls, spiny mice and zebrafish.
“Zebrafish quickly became my favorite animal,” said Mokalled, who heads a lab funded by the National Institutes of Health (NIH) in the Department of Developmental Biology. “If their spinal cord is severed, the fish become paralyzed for a few weeks before their cells repair the injury and restore their ability to swim. Almost every aspect of regeneration we’re trying to achieve in humans is already happening in zebrafish.”
Her groundbreaking research has found that spinal cord injury in humans causes scarring of the glial cells, members of the nervous system that are important in maintaining brain function. The damage prevents the regrowth of nerve cells in the spinal cord, causing paralysis. In contrast, glial cells in zebrafish mobilize to form a bridge across the injured spinal cord, leading to its regeneration and restoration of movement.
In her lab, Mokalled and her team are implementing what they learned about zebrafish regeneration to spur spinal cord repair in mice. Eventually, she aims to apply her findings to engineer spinal cord repair in humans.
“The answers are out there,” she said. “We just must look for them.”
Deborah Parks, MD
Deborah Parks, MD, a professor of medicine and director of clinical operations in the Department of Medicine’s Division of Rheumatology, was recognized as an exceptional clinician who has provided more than 35 years of skilled patient care. Parks is a highly respected and empathetic physician who has become known as “a physician’s physician.” When she began residency, the curriculum focused primarily on physiology, anatomy, pharmacology, scientific research and emerging technologies in patient care. And while these are all essential, Parks quickly learned that one of her most powerful tools was plain language.
Instead of using unfamiliar medical terminology such as arthralgia, myalgia or joint effusion, Parks spoke to patients about their joint pain, muscle pain and swollen joints.
“Listening to the patient is also key,” said Parks, who treats patients at Barnes-Jewish Hospital. “Discussing their health should be a conversation, not a lecture.”
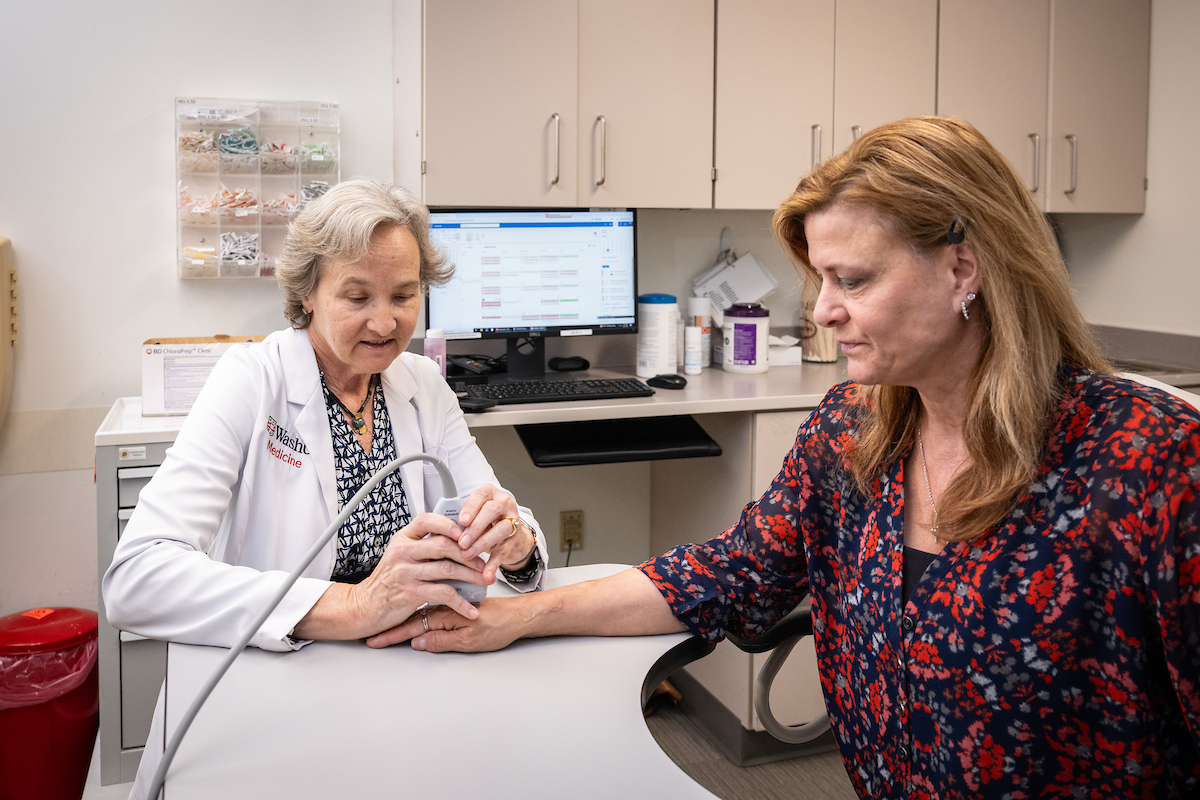 Carol Green/WashU Medicine
Carol Green/WashU MedicineFor decades, Parks has trained medical students and residents to prioritize lay language and listening in their patient interactions. She also taught them the importance of eye contact, empathy, compassionate gestures and noting personal details.
“We want to embed into our trainees who go on to practice across the U.S. and around the world that clear communication is essential to making patients feel valued and obtaining the best health outcomes,” said Parks, who has treated generations of families and often receives visits and notes from former patients. “My philosophy is to treat each patient the way I would want a physician to care for a family member or friend.”
Read more about the 2026 Dean’s Impact Award winners on the WashU Medicine Office of Faculty Promotions and Career Development website.